
Surgical interventions may be required if evidence of delayed union or nonunion exists. Weight-bearing status can advance as tolerated by pain. Nondisplaced dancer’s fractures and other fractures of the fifth metatarsal shaft and neck receive the same treatment as nondisplaced zone 1 injuries. The medullary cavity must be curetted or drilled until all the sclerotic bone has been removed and the medullary canal reestablished prior to inserting the donor graft. 
The bone grafting inlay technique requires removing a 0.7 by 2.0 cm rectangular section of bone at the fracture site and replacing it with an autogenous corticocancellous bone graft of the same dimensions taken from the anteromedial distal tibia. Surgical options include intramedullary screw fixation, bone grafting procedures, or a combination of the two. High-performance athletes or individuals with Torg Type II or III fractures may require surgical interventions. A trial of conservative management with non-weight bearing in a short leg cast may be the initial therapy however, immobilization for up to 20 weeks may be necessary before there is observable radiographic union, and even then, nonunion development is not uncommon. Surgical management of high-performance athletes minimizes the risk of nonunion and prevents prolonged restriction from physical activity.ĭiaphyseal zone 3 stress fractures paint a more complicated picture for the patient and physician. There are many forms of surgical interventions, including intramedullary screw fixation, tension band constructs, and low-profile plates and screws. Indications for surgical interventions include the high-performance athlete, the informed patient who elects to proceed with surgical treatment, or displaced fractures. The physician may advance weight-bearing status as radiographic evidence of bone healing appears. Nondisplaced zone 2 injuries, or Jones fractures, may also be treated conservatively with 6 to 8 weeks of non-weight bearing in a short leg cast. Fractures involving 30% of the articular surface or with an articular step-off over 2 mm have treatment with open reduction, internal fixation, closed reduction, and percutaneous pinning or excision of the fragment. Progression to weight-bearing as tolerated can initiate as pain and discomfort subside over 3 to 6 weeks. Nondisplaced zone 1 injuries can be treated conservatively with protected weight-bearing in a hard-soled shoe, walking boot, or walking cast. Treatment decisions have their basis on the anatomic zone of injury, the social and medical history of the injured patient, and evidence of radiographic signs of healing. A vascular watershed area exists in zone 2, contributing to the high nonunion rates seen with these fractures. Metaphyseal arteries and diaphyseal nutrient arteries provide the blood supply to the fifth metatarsal base. Additionally, a patient may sustain a shaft fracture greater than 1.5 cm distal to the tuberosity, a long spiral fracture extending into the distal metaphyseal area, the so-called dancer's fracture, or a stress fracture of the metatarsal.Ĭlassification of these fractures is crucial to making management decisions. 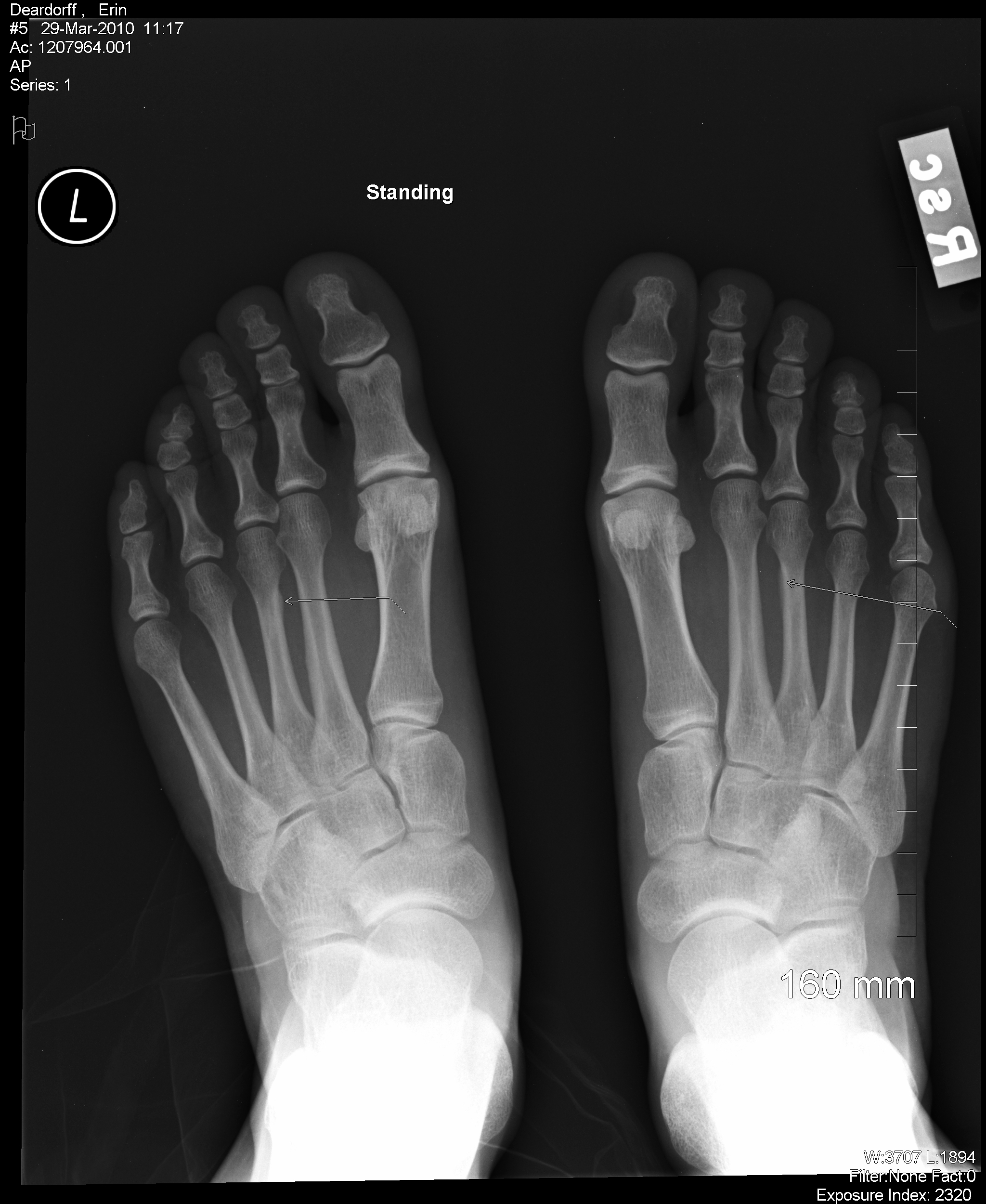
Fractures through zone 1 are called pseudo-Jones fractures, and fractures through zone 2 are referred to as Jones fractures. Nevertheless, it is critical that the clinician recognizes all injury patterns of the fifth metatarsal and initiate the appropriate treatment plan or referral process to avoid potential complications.Ĭlassified by Lawrence and Bottle, the base, or proximal aspect, of the fifth metatarsal is broken up into three anatomical zones: zone 1, the tuberosity zone 2, the metaphyseal-diaphyseal junction and zone 3, the diaphyseal area within 1.5 cm of the tuberosity. Since orthopedic surgeon Sir Robert Jones first described these fractures in 1902, there has been an abundance of literature focused on the proximal aspect of the fifth metacarpal due to its tendency towards poor bone healing. Fractures of the fifth metatarsal are common injuries that must be recognized and treated appropriately to avoid poor clinical outcomes for the patient.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
